Pancreatic Cancer Surgery
Listed below is the step by step procedure of pancreatic cancer surgery:
- What is Pancreatic Cancer Surgery?
- Why is Pancreatic Cancer Surgery Required?
- Pre-operative Preparation
- Day Before Surgery
- Procedure Day
- Methods/Techniques of Pancreatic Cancer Surgery
- Post Procedure
- Risk Factors and Complications
What is Pancreatic Cancer Surgery?
Pancreatic cancer surgery is an effective way to deal with cancer associated with pancreas. Pancreatic cancer occurs when the pancreatic cells grow abnormally and develop abnormal structure and function. These uncontrolled multiplication of cells results in forming a mass called tumor.

There are various surgical methods that are used to eliminate such cancerous tumors as well as cancer cells from your body. Due to rapid multiplication of cancer cells, cancer can also affect their neighboring cells and tissues, gradually growing and spreading to other parts of the body. All these factors necessitate surgery for treating the patient.
Why is Pancreatic Cancer Surgery Required?
Pancreatic cancer surgery serves as one of the best way to treat pancreatic cancer. Most early stages of cancer can be cured completely with surgery. Although, pancreatic cancer cannot be easily detected at its early stage. By the time a patient is diagnosed with pancreatic cancer, the disease has already reached its advanced stage. Due to such reasons, a surgery could be necessary to remove your entire pancreas.
Surgery can potentially cure your body from pancreatic cancer. It can also be used as a palliative measure in order to improve the quality of patient's life. A palliative surgery is found helpful in relieving patients from the symptoms of pancreatic cancer.
Pre-operative Preparation
There are many important measures conducted before performing the main surgery procedure in order to learn certain aspects about the patient's health condition. Pre-operative steps involve various tests and methods that are needful to decide the best surgery method for your cancer condition. This would also include scheduling the day for your surgery.
Tests Various pre-operative tests include:
General examination- Doctor examines your skin and eyes to check for symptoms like jaundice that can be caused if you have pancreatic cancer. Patients are also asked about their medical history.
Imaging Tests
- Computer Tomography (CT) Scan- CT scan can gives multi-dimensional images of pancreatic cancer present within your body. This is required for the doctor to learn about various aspects of pancreatic cancer that are needful before the surgery.
- Positron Emission Tomography (PET) Scan - A PET scan is usually combined with CT scan. A PET scan gives multi-colored images of internal tissues of pancreas and nearby organs. Your doctor requires these images to check the extent to which your pancreatic cancer has spread and where the surgeries are required.
- Ultrasound - Ultrasound process includes using sound waves for imaging pictures of the cancerous tumors present within or around your pancreas. This test gives your doctor the location and size of tumor. Based on these two factors, the doctor decides about which surgical technique will be more effective.
Biopsy and Tissue Tests
- Biopsy- The removal of small amount of tissues from your internal body structures is known as biopsy. Here, pancreatic tissue samples are sent to the pathology labs and examined under the microscope to detect the presence of cancer and the extent to which it has spread. Location of cancer helps the doctor select the site of surgery.
- Molecular testing of tumor- Doctors take your blood samples or tissue sample in order to detect and identify certain genes, proteins or other factors unique to a tumor. These factors are called as biomarkers. If biomarkers are detected in certain tissue bodies, they can be surgically removed.
Day Before Surgery
Planning for a pancreatic cancer surgery involves discussing with your doctor about what are the steps to follow prior to your surgery.
Doctor will explain you in detail about the entire surgery procedure. Every case of a cancer patient is unique. Hence, before going for the surgery, doctors will discuss the pros and cons of the pancreatic cancer surgery with their patients.
Some doctors can prescribe you certain drugs that you must consume in your pre-operative period.
There are some precautions to be followed before your go for a surgery. Such precautions include:
- Avoid intake of alcoholic drinks
- Avoid consuming any forms of tobacco
Procedure Day
On the day of your pancreatic cancer surgery, you may have to fast for some hours before going for the procedure.
Your doctor will conduct your physical check up to see if your sugar level, pH level and blood pressure is normal. If there are any abnormal changes in these health factors, your surgery can be re-scheduled.
Initially, patients are sedated before starting with the surgery procedure. A pancreatic cancer surgery will require making incisions in your abdominal region. Incisions can also be made in other parts of your body if cancer has affected those areas. The size of incision made, depends on the method of surgery being used. For laparoscopic approaches, the size of the incisions are very small. Tissue bodies affected with cancer are removed. For advanced stages of pancreatic cancer, the team of surgeons can remove the entire pancreas from your system.
After executing pancreatic cancer surgery process, incisions are stitched or stapled back. To avoid bleeding and infections, nurses apply anti-septic on those areas and cover them with cotton gauges. Also, cotton dressing is done in those places so that the stitches remain intact.
Some patients are injected with certain medications that make them unconscious, allowing their body to rest after the surgery. Doctor will also monitor your vitals after the surgery. If there is a lot of bleeding observed during your surgery, your body's vital conditions can show some changes. At such times, there can be a need of transfusion of blood into your system.
Methods / Techniques of Pancreatic Cancer Surgery
To determine which type of surgery is best for the cancer patient, the doctor requires to know about the stage of cancer. Imaging tests do not precisely tell you about the stage of the cancer. At such times, a laparoscopy is done before conducting surgery in order to determine the extent of cancer and whether it can be surgically removed.
For a laparoscopy procedure, initially your surgeon makes few incisions, in your abdominal area. A thin, long, flexible tube is inserted through one of the incision, called as a laparoscope. A laparoscope contains a camera, light and some surgical tools attached to its end. Through the video camera, the surgeon can take a look inside the abdomen, pancreas and neighboring tissue bodies. Samples can also be collected for biopsy purpose to learn about the extent to which cancer has spread.
There are two general types of surgeries that can be implemented for pancreatic cancer. These are:
- Potentially curative surgery
- Palliative surgery
When the results of the diagnostic tests show that it is possible to remove the entire cancer, this surgery technique can be used.
Removing a section of your cancer does not help the patients live longer. Hence, this surgery is performed to remove entire cancer from your body. However, if during the surgery, the surgeon finds that cancer has affected some unnoticed areas too, he/she will stop the surgery and perform a palliative surgery to prevent symptoms. This is done because the planned operation can include major side effects that can take longer recovery time.
Most surgeries can offer complete cure, but some might not lead to a cure, even after removal of visible cancer. This is because of some unidentified cancer cells that can later grow into new tumors which are hard to treat.
Curative surgery is mainly done when the cancer exists in the head of pancreas. This cancer is mainly present near the bile duct. If found early enough, it can be removed.
Whipple procedure (pancreaticoduodenectomy)- This is a surgical procedure used to remove exocrine pancreas affected with cancer. It is also used to treat pancreatic Neuroendocrine Tumors (NETs). In this surgery, doctor can remove the head or the entire pancreas along with small intestines, lymph nodes near the pancreas, part of bile duct, gallbladder and sometimes even a part of your stomach.
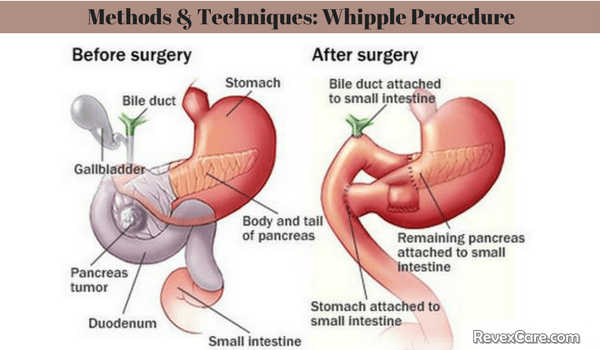
The remaining part of your bile duct and pancreas is attached to the small intestine so that digestive enzymes and bile can enter the small intestine. Small intestine or part of your stomach can be reattached in order to let the food pass through your digestive tract.
Distal Pancreatectomy- In this surgery, the surgeon discards the tail and some section of the body of pancreas. The spleen is also removed. The spleen functions to fight infections. If removed, the risk factor of acquiring bacterial infections increases. This can be treated later by vaccines. If spleen is removed, medicines have to be taken to maintain immunity at the optimum levels. This operation is usually conducted to treat pancreatic NETs found in the tail or other parts of the pancreas.
Total Pancreatectomy-

This surgical method is performed for removing the entire pancreas, along with gallbladder, small intestine, spleen and part of your stomach. This operations is used less often as it does not give any major advantage over removing the entire pancreas, and also it includes major side effects. Living without pancreas is possible but there wont be any production of enzymes and hormones that maintain blood sugar levels. Hence, such patients develop diabetes. Also, such patients require to consume pancreatic enzyme pills to digest some food items. Vaccines are given before the spleen removal operation. After spleen is removed, dose of medicines should be taken to maintain immunity level.
2. Palliative surgeryWhen the scanning tests show that cancer has spread widely and cannot be removed completely, this surgery is suggested by the surgeon. It is used to prevent further complications like a blockage in the intestine or duct. This is not a curative surgery.
Pancreatic cancer progresses quickly. When cure is not possible, the doctor might go for a less extensive, palliative surgery. This is a bypass surgery that aims to help prevent or relieve the symptoms.
When cancer grows in the head of the pancreas, it blocks the bile duct. This causes pain and digestive disorders. There are two methods to get relief from such bile duct blockages:
Placement of stents- To get rid of blockages in your bile ducts, a small metallic tube, called stent is placed inside your bile duct to open it up. This procedure is carried under sedation using an endoscope. It is usually a part of Endoscopic Retrograde Cholangio-Pancreatography (ERCP) operation. Here, endoscope is passed through your throat into your small intestine. The stent can also be placed in the duct using Percutaneous Transhepatic Cholangiography (PTC).
The stent helps the duct open up, but within months this stent can get clogged and may require to be cleared or to be replaced. Larger stents can be used for clearing blockages in the small intestine.
Bypass surgery- The second method for relieving from a bile duct blockage is going for a bypass surgery. This method involves bypassing the pancreas and re-routing the flow of bile from bile duct into the small intestine directly. This surgery can be done by making larger incisions or through laparoscopic approach.
Placing a stent into your bile duct is easier than a bypass surgery. Although, bypass surgery has some advantages that include:
- Long-lasting relief than the stent, which may require replacement or cleaning after some months
- For some reason, if the stent cannot be placed, this is an alternative option to remove the blockage.
- In this surgery, surgeons may cut some nerves or inject it with alcohol that may relieve patients from pain caused due to pancreatic cancer.
Sometimes, a gastric bypass can be made, where stomach is disconnected from the duodenum and attached to the small intestine. This is done if there are chances of the duodenum to get blocked due to cancer.
Apart from the above mentioned procedures to treat pancreatic cancer, a process known as Enucleation is also adopted.Enucleation is a surgical mechanism, where just the tumor is removed. This is done if the pancreatic NETs are smaller in size. A laparoscopic methodology can be used in this surgery.
This operation is mainly conducted to treat insulinoma (tumor present in the pancreas that secrete excessive insulin), as it contains tumor of benign (non cancerous) type. Also, pancreatic cancers like small gastrinomas (tumor present in pancreas that produces excessive gastrin, leading to ulceration) and other NETs may also be treated using enucleation. In some cases, the surgeon may remove your duodenum as well as the lymph nodes around the pancreas, if they are found affected.
Post Procedure
Post procedure care is very important for a faster and better recovery. PrecautionsAfter pancreatic cancer surgery, there are a lot of things that the patient must keep in mind. Precaution is one of them. Patients should take some necessary precautions for a better healing. Necessary precautionary measures include:
- Avoid consumption of alcohol while you are under medications
- Do not lift heavy objects, they can put pressure on your stitches
- Do not perform rigorous activities
- Change your bandages from time to time to avoid infections
Recovery at Hospital
After your pancreatic cancer surgery is successfully performed, you will be taken to general room so that you rest for some hours. Going through a surgery is quite painful internally as well as externally. You will be given some injections, medicines or pain killers that will help you sleep.
After some hours, your doctor checks your vitals. Some surgeries experience heavy blood loss. In such a case, blood transfusion can be done while you are asleep. Also, glucose can be transfused into your system if required. If there is any abnormality in your vital signs, necessary steps can be taken.
Physiotherapy can begin during your hospital stay. Therapists can teach you exercises that you can perform to keep your body healthy. Meditation and yoga can also be included during these sessions. These set of exercises can be later continued at home.Once your health status is considerably better, you will be allowed to go home. Your doctor will make a diet chart and also provide you with some medications that you should consume on time.
Recovery at HomeYour body must get proper amount of sleep while it is under recovery. Patients must continue performing the recommended exercise, meditations or yoga.
Advanced stages of pancreatic cancer may require removal of your pancreas entirely. Hence, surgery can be performed to remove it. Living without pancreas is possible, but there wont be any production of enzymes and hormones that maintain blood sugar levels. Hence, such patients develop diabetes. Also, such patients require to consume pancreatic enzyme pills to digest some food items.
Consuming healthy diet is very necessary to keep your body fit during recovery period. After your cancer surgery your body's tolerance level reduces to some extent. Hence, for strong medicines, a healthy diet can make your body bearable for it.
Follow-up AppointmentsAfter the pancreatic cancer surgery, follow-up appointments are a must. It shows whether your recovery process is going smoothly. If you experience any trouble or side effects, you can let your doctor know about it. There can be some tests involved during follow-up checkups to ensure that your health condition is fine.
Life After the SurgeryA pancreatic cancer patient who gets his pancreas entirely removed, suffers from diabetes afterwards. Such patients have to take diabetes medicines for life time and restrict themselves from consuming certain food items. Your doctor will help your regarding this problem.
Risk Factors and Complications
Even under best circumstances, there can be risks involved for a pancreatic surgery.
Risks of potentially curative surgery include:
- Leakage from the attachments made
- Bleeding
- Trouble while digesting certain food items
- Loss in weight
- Diabetes
- Infections
- Trouble emptying your stomach after food intake
- Changes in the bowel movements
Risks of palliative surgery include:
- Infections
- High Temperature
- Shivers
- Pain (remains for some few days)
The above article enlightens us about pancreatic cancer surgery, its pre-procedure preparations and other necessary related aspects. Any unclear points can be discussed with your oncologists.


